The nursing profession is currently undergoing massive changes—and there are some telling nursing industry trends from this past year that point toward more changes and opportunities on the horizon. Learn more about the nursing industry as we take an overview of its state in 2022.
Nursing is one of the most critical professions not only in the United States but around the world. The Covid-19 pandemic proved the worth of nurses on the frontlines; in the face of their own exposure to the disease, nurses continued to provide vigilant care. However, the pandemic illuminated some dire nursing industry trends and kicked off others.
The roles and responsibilities of the nursing care team, whether registered nurses (RNs), licensed practical nurses (LPNs), certified nursing assistants (CNAs), and licensed vocational nurses (LVNs), are vast and include assessment, care planning, patient advocacy, collaboration with the indiscipline team, evaluation of the social determinants of health, and education across the continuum of care. And as advanced practice registered nurses (APRNs) and nurse practitioners (NPs), they diagnose diseases and prescribe medications.
Nurses are needed everywhere, from bustling metropolises to remote towns. Opportunities for qualified nurses are always expanding; however, the stress of the pandemic took its toll on many nurses who subsequently left the profession, many due to early retirement, fear of taking the disease home to loved ones, and emotional/mental toil from the many aspects of the pandemic. As such, the profession is undergoing massive changes—and some telling nursing industry trends from this past year point toward more changes and opportunities on the horizon.
1. The Nursing Staffing Shortage Will Increase
Though the demand for nurses is great, one of the most significant nursing industry trends indicates that there is also a growing nursing shortage. This is a serious problem in the face of a growing need for direct patient care.
Fewer nurses must care for more patients—reducing the quality of care and decreasing the quality of health outcomes. This shortage is exacerbated by healthcare workers, with nursing assistants, care providers, and food services staff in low numbers, resulting in added workloads on top of their existing primary nursing.

This nursing shortage isn’t exactly new. It’s been building well before the pandemic—back in 2017, the Health Resources and Services Administration predicted a need for a million new nurses in the next ten years. The reason for such dire numbers is the large demographic of Baby Boomers aging and living longer. The average age of nurses is 52 years old, and an influx of traditional bedside nurses leaving for flexible schedules, more pay, or to advance their careers.
With age comes changes in general health and mobility; long-term care facilities that house the elderly have faced several challenges, especially the complexity of patient care and budget-cutting measures.
When the pandemic struck, long-term care facilities were hit especially hard since the elderly were more vulnerable to Covid-19. During 2020, 96% of assisted living communities and 99% of nursing homes in the U.S. were short-staffed.
The pandemic also spurred what has been termed the “Great Resignation,” when workers voluntarily quit their jobs in droves. Those leaving jobs were not just part-time workers or those in low-wage positions; high-earning, well-educated professionals also left in large numbers.
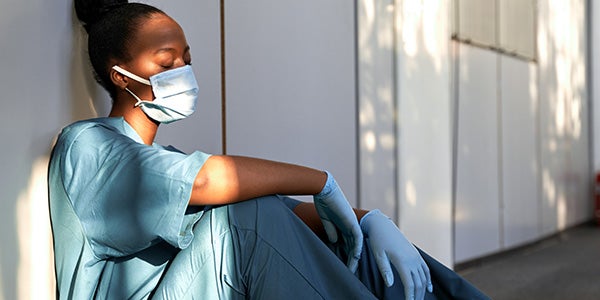
Healthcare workers—especially nurses on the front lines of the pandemic—faced exhaustion, burnout, and trauma. Unlicensed assistive personnel were also leaving the profession in large numbers, increasing the workloads of RNs. The rate of nursing turnover has grown from 17% in 2017 to 29% in 2022—with many planning to leave not just direct patient care but the profession entirely.
Unfortunately, the number of nurses graduating hasn’t been able to keep up with the growing need. From 2016 to 2019, nursing licensures experienced a 4% growth. But by 2020, growth had diminished to 1%.
There are some remedies, many of which have been around for a long time, while others came out due to the pandemic. All healthcare settings are being forced to redesign the delivery of care model due to healthcare worker shortages.
One of the most urgent changes is the adoption of flexible scheduling. This lets nursing staff choose the shifts that work best for them. Scheduling software can simplify this process, relieving managerial burdens because nurses can do this themselves. Flexible scheduling is a great incentive for recruiting new workers and keeping seasoned ones.
Cross-training non-direct care staff can help ease the burden of RNs. Having these workers handle tasks that are indirectly related to patient care—such as stocking supplies or making beds—can let nurses concentrate on the health needs of their patients.
Innovative team models can also reduce the burden that nurses experience providing direct patient care. The usual model sees the RN caring for multiple patients with help from non-direct care staff. A team model puts the nurse as a team manager who supervises other staff to provide direct care.
Finally, providing professional development training focusing on mental health can give nurses tools to avoid burnout and manage stress and trauma. Self-care strategies are vital for the well-being of the nursing staff.
2. Nurses Will Make More Money
While the first of these nursing industry trends might be bad news, this is a positive for nurses everywhere. The shortage of nurses—and the growing demand for them in direct patient care—has hospitals, clinics, long-term care facilities, and doctor’s offices boosting salaries. Current nursing workers of all ranges of education and certification saw pay increases in 2021.
One of the primary reasons nursing salaries are rising is the Covid-19 pandemic and what it revealed about the profession. Nurses face danger every day, especially when dealing with infectious diseases. Wages must reflect that risk by increasing.
According to some industry sources, another driving force for salary increases is the extreme inflation of agency rates. As healthcare organizations made every effort to provide safe, quality care despite having a census beyond bed capacity, the staffing agencies raised their rates drastically.
Wages also need to account for additional training. A CNA who goes back to college to complete a degree to become an RN should receive more money. The same applies to RNs getting specialty training to be surgical or psychiatric nurses.
In addition, the different needs of diverse working environments may have more risk or more specialized duties. For example, traveling nurses work in a variety of locations with a range of different duties. They must be flexible and adaptable and thus receive higher salaries on average.
3. Increasing Demand for BSN Programs
One of the most interesting nursing industry trends is that though veteran nurses are voicing their desire to leave the field, many new students are entering Bachelor of Science in Nursing (BSN) programs.
In 2021, The American Association of Colleges of Nursing (AACN) reported enrollment in BSN programs had increased by 3.3% and Doctor of Nursing Practice by 4%. This is a change since many nurses begin their careers as CNAs, work for a while, obtain state licensure as an RN, and then return to receive a BSN. The AACN reported enrollment numbers down for more advanced degree (Master's and Ph.D.) programs.
Every year, though, qualified students are refused acceptance at many nursing schools. In 2021, 91,938 applications were rejected, the most since 2002. The main barriers have been university budget cuts, lack of classroom space and faculty, and too few clinical placement sites. But despite those numbers, nursing students are still applying, knowing that the nursing profession is a stable and lucrative one.
4. Support for Nurses’ Mental Health Will Increase

The Covid-19 pandemic drew attention to the long-term mental health issues nurses experience. Nurses faced trauma daily, helping their desperately ill patients and witnessing how the pandemic affected families.
It was devastating for many nurses to care for patients for weeks, only to come in their next shift to be told the patient had finally succumbed after their long battle. In the past, nurses could leave work at home, but the pandemic also impacted their life at home. Their workplace stress is compounded with worries about their families' health and needs at home.
These conditions spotlighted one of the most enduring nursing industry trends: the stress, exhaustion from working long shifts, and depression nurses have felt for decades. Increases in wages by the healthcare industry were a long overdue response. However, these vital workers deserve more support.
A 2022 survey revealed that nurses' well-being and mental health had declined by 26%
from pre-Covid states. Nurses reported burnout, depression, and compassion fatigue since the pandemic began. Most alarming, 10% of nurses—more than twice the prevalence in the general adult population—reported suicidal thoughts.
An additional 95% reported that they felt that the healthcare industry didn’t care about their mental health or that there were no remedies in place. Further, nurses were reluctant to share their feelings of acute mental health issues for fear of losing their jobs, confidentiality issues, or making no effort to help.
Mental health problems in nursing aren’t new. Compassion fatigue and physical exhaustion lead to poor patient outcomes and decreased nursing performance. This, in turn, leads to nurses feeling decreased self-esteem and even alienation from coworkers. Before the pandemic, only trauma or combat nurses experienced extreme burnout and post-traumatic stress disorder (PTSD). Covid-19 allowed nearly all nurses to experience some kind of trauma.

Exhaustion, constant stress and PTSD often lead to suicide. However, the National Violent Death Reporting System that the CDC compiles showed that even two decades before the pandemic, nurses had reported significantly more mental health issues before they took their own lives. They had more serious job, physical health, and substance abuse issues. Nurses often remained silent about their turmoil, seeing how a negative physical or mental health issue affected patients’ work and social experiences.
There are some strategies and programs that can support nurses’ mental health. Flexible scheduling, again, is a way to spread out work and stress. Wellness stipends and access to fitness facilities also help manage workplace stress.
Providing trauma-informed groups can help nurses safely express their feelings without being stigmatized or ostracized. Offering stress-relieving wellness classes such as meditation and yoga can alleviate the pressures. One hospital even had nurses work with a musician to write songs about their feelings.
Whatever strategies are employed, the healthcare industry must look at these disturbing nursing industry trends and create a culture in which nurses are appreciated and supported. Nurses need to feel as safe talking about their mental health issues as they would about having tired feet. In addition, more effort needs to be made to reduce the stigma attached to mental health issues.
Another area that affects nurses is moral suffering, especially during the pandemic, about treating critically ill patients and deciding who would get care with limited resources. John Hopkins University created the Mindful Ethical Practice and Resilience Academy to help nurses with burnout and moral suffering. Six intensive workshops over 12 weeks focused on moral resilience, moral agency, moral sensitivity, moral discernment and reasoning, and moral actions. The program has produced positive results, significantly reducing depression and anger, and quitting intentions.
5. The Rise of Telehealth Nursing

Telehealth nursing is one of the most promising nursing industry trends. Telehealth has existed in remote areas, such as small mountain villages in Alaska, where flying in a physician or a home health nurse proves difficult. Covid-19 led to widespread adoption since patients could be seen via video call, and a determination could be made whether to go to the ER. Telehealth nursing can be available on computers, tablets, and even smartphones. Some physicians in direct patient care or concierge medicine see patients via Zoom to check their progress.
Patients and healthcare professionals alike benefit from telehealth nursing. Patients don’t have to travel to talk to a nurse or be exposed to other illnesses in a crowded doctor’s office or ER. Nurses don’t have to travel either, except for more seriously-ill patients.
Nurses make acute observations about a patient’s mental state and physical health through body language and how they make conversation. This determines whether the nurse needs to make an in-home visit or the patient should come to a doctor’s office. Often, nurses can diagnose lower-risk conditions, offer home treatment suggestions, and educate patients.
Formerly, telehealth was conducted through private agencies. Over the last two decades, it has become an extension of many clinics, hospitals, and healthcare plans. The American Telemedicine Association estimates that half of all healthcare services will be provided through telehealth within the next five years.
The need for nurses will only continue to increase since nurses provide meaningful support and guidance to patients. Telehealth improves patients’ access to care and contributes to successful health outcomes.
The service can help ease the nationwide nursing shortage by providing more attentive and better direct care in a calmer environment than a busy hospital or clinic. Telehealth nurses can focus on patient care, taking more time to build rapport and trust. Access to a caring nurse creates patient bonds, often securing medication and treatment adherence and better patient outcomes. Therefore, nurses feel more job satisfaction.

Nurses can prepare for telehealth jobs by earning an associate degree in nursing or a BSN from an accredited program. They must pass a state licensure exam and obtain experience in direct patient care. Telehealth nurses don’t need certification, but it does offer an advantage in the job market.
For seasoned nurses seeking a job change, continuing education programs can offer telehealth skills in technology. New advances in medical technology have become useful additions to acute observation and compassion. Nurses can use peripheral devices such as Bluetooth-enabled stethoscopes and cameras, and remote glucose meter monitors.
Planning for the Future of Nursing
Many of these nursing industry trends are serious but also encouraging. The healthcare industry must change its culture to address nurses' mental health and physical needs to reduce the number of nurses leaving the profession. New technologies to help patients will attract new and seasoned nurses into these promising new fields. Increased salaries, signing bonuses, and loan repayment incentives are proven recruitment tools to fill the nursing shortage.
Healthcare organizations must implement new programs and strategies to help nurses who require financial experts. Having a reliable financial partner like Illinois Bank & Trust, a division of HTLF Bank with deep industry insights can help organizations navigate the challenges and uncertainties of the future. If you are a healthcare operator, provider, or investor, contact Illinois Bank & Trust, a division of HTLF Bank today to explore solutions that can help you fund new nurse staffing strategies.







